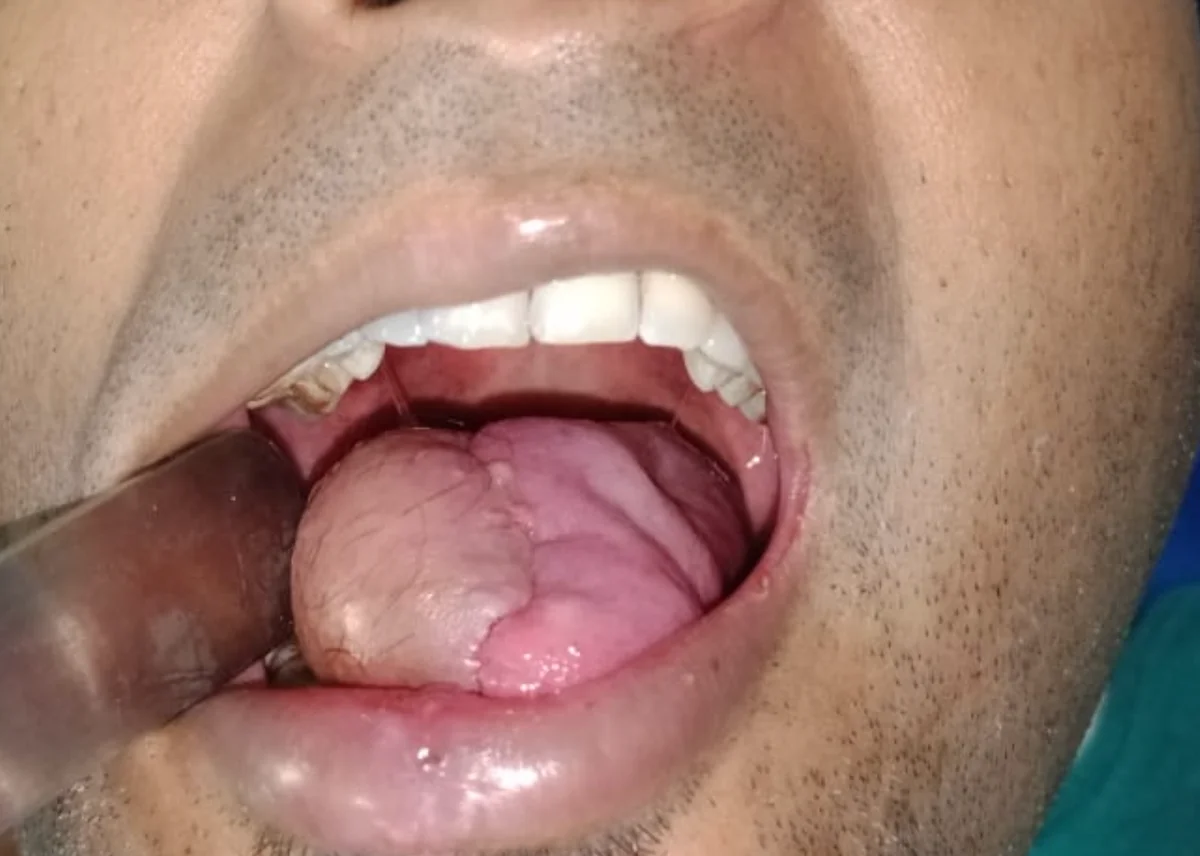
Tongue cancer management is a multidisciplinary process. Surgery provides the primary oncological treatment — tumour excision and neck dissection — but adjuvant treatment coordination with radiation oncology and medical oncology is essential for patients with high-risk pathological features.
After surgery, the removed specimen is analysed by the histopathologist to assess: surgical margin status (clear, close, or involved), depth of invasion, perineural invasion, lymphovascular invasion, number of positive lymph nodes, and whether extranodal extension is present. These pathological features guide the multidisciplinary team decision on adjuvant radiotherapy or chemoradiotherapy.
Maxillofacial Surgeon Primary surgical resection, neck dissection, and free flap reconstruction
Radiation Oncologist Post-operative radiotherapy or chemoradiotherapy planning and delivery
Medical Oncologist Concurrent chemotherapy for high-risk pathological features
Speech & Swallowing Therapist Rehabilitation of speech and swallowing function post-surgery and post-radiation