Non-Healing Ulcer
A mouth ulcer that does not heal within 3 weeks is the most common early sign of oral cancer. Any persistent ulcer must be evaluated.
Oral cancer is one of the most common cancers in India. Early detection dramatically improves outcomes. If you have a mouth ulcer or abnormal patch that has not healed in 3 weeks, seek specialist evaluation now.
A mouth sore that has not healed in 3 weeks — even if painless — requires medical evaluation. Early stage oral cancers are often painless. Pain is usually a late symptom.
Oral cancer refers to malignant tumours arising from the lining of the mouth. The most common type is squamous cell carcinoma (SCC), which develops from the squamous cells that line the inner surface of the lips, tongue, floor of mouth, gingiva (gums), buccal mucosa (inner cheek), palate, and oropharynx.
India has one of the highest incidences of oral cancer in the world, largely attributed to the widespread use of tobacco, areca nut (betel nut), and related products. Oral cancer accounts for a significant proportion of all cancers in India, particularly in states where tobacco and areca nut chewing are prevalent.
The most common sites for oral cancer are the tongue (particularly the lateral border — the sides of the tongue), the floor of the mouth, and the buccal mucosa (inner cheek lining). Less common sites include the hard palate, gingiva (gum), and lip.
Critically, oral cancer detected at an early stage (Stage I or II) is associated with significantly better outcomes than advanced stage disease. This makes early recognition of warning signs, and prompt specialist evaluation, among the most important factors in improving oral cancer outcomes.
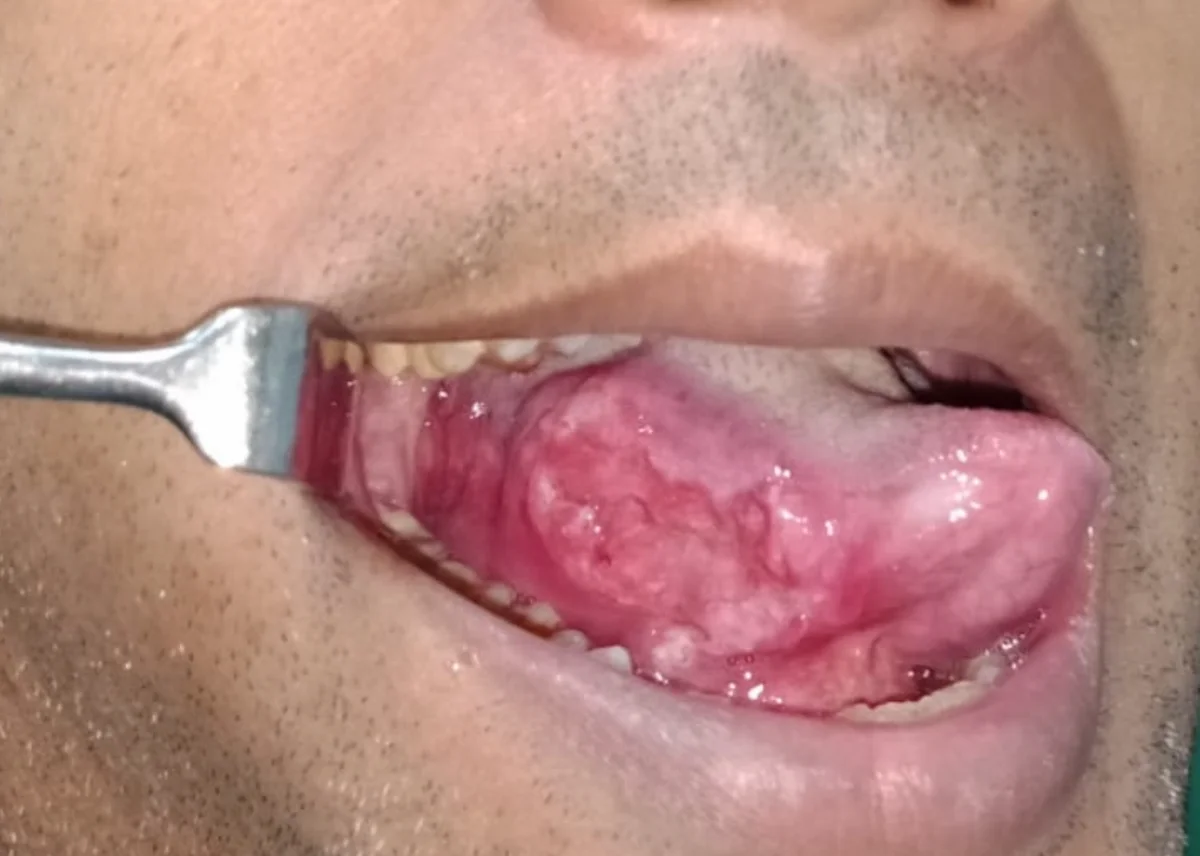
These symptoms do not always mean cancer — but any of them lasting more than 3 weeks requires specialist evaluation. Earlier evaluation means better outcomes.
A mouth ulcer that does not heal within 3 weeks is the most common early sign of oral cancer. Any persistent ulcer must be evaluated.
White patches on the tongue, gum, or inner cheek that cannot be wiped off. Some white patches are premalignant and require biopsy.
Red velvety patches in the mouth carry a higher risk of malignancy than white patches and require prompt biopsy.
Persistent difficulty or pain with swallowing (dysphagia) may indicate a tumour in the mouth, tongue, or throat affecting swallowing mechanics.
An enlarged lymph node in the neck that persists for more than 3 weeks may indicate spread of oral cancer to the cervical lymph nodes.
Persistent numbness, tingling, or altered sensation in the lip, tongue, chin, or cheek without apparent cause may indicate nerve involvement by a tumour.
Understanding risk factors is the first step in prevention. Reducing or eliminating modifiable risk factors significantly lowers the probability of developing oral cancer.
Smoking cigarettes, bidis, or using chewing tobacco is the single largest risk factor for oral cancer. Risk increases directly with amount and duration of use. Smokeless tobacco products are particularly associated with cancers of the buccal mucosa (cheek lining) and gingiva.
Chewing areca nut (supari) with or without betel leaf and tobacco is a major risk factor for oral cancer and oral submucous fibrosis, particularly prevalent in India. Gutka and pan masala products with areca nut carry significant carcinogenic risk.
Alcohol use independently increases oral cancer risk, and the combination of tobacco and alcohol has a synergistic (multiplicative) rather than simply additive effect on cancer risk.
Human papillomavirus (HPV), particularly HPV-16, is associated with oropharyngeal cancers (base of tongue, tonsil). HPV-associated oral cancers tend to affect younger patients without traditional risk factors.
Chronic irritation from sharp or broken teeth, ill-fitting dentures, or poor oral hygiene may contribute to localised tissue changes that increase cancer risk when combined with other risk factors.
OSMF is a pre-malignant condition strongly associated with areca nut chewing. It causes progressive fibrosis of the mouth lining, restricted mouth opening, and carries a significant risk of malignant transformation into oral cancer.
Seek immediate specialist evaluation if you have any of the following:
Accurate diagnosis and staging is essential before any treatment decision is made.
Thorough examination of the entire mouth, tongue, floor of mouth, palate, and oropharynx. Palpation of the neck for lymph nodes. Assessment of mouth opening range and swallowing.
A tissue sample taken from the suspicious area under local anaesthesia and sent for histopathological examination. Biopsy is the only definitive method to confirm or rule out cancer.
CT scan and MRI of the head and neck to assess tumour size, depth, bone involvement, and lymph node status. OPG for jaw bone assessment. PET-CT for distant metastasis screening in advanced cases.
Staging (Stage I–IV) is determined by tumour size, depth of invasion, lymph node involvement, and distant spread. Staging guides treatment planning, which is discussed in a multidisciplinary setting.
Surgery is the primary treatment for most oral cancers. The goal of surgery is to remove the tumour completely with clear margins (a border of normal tissue around the tumour), to give the best chance of cure and prevent local recurrence.
For early-stage oral cancer, surgery alone may be curative. For more advanced cancers, surgery is often combined with radiation therapy, chemotherapy, or both (multimodal treatment), typically coordinated with a multidisciplinary oncology team.
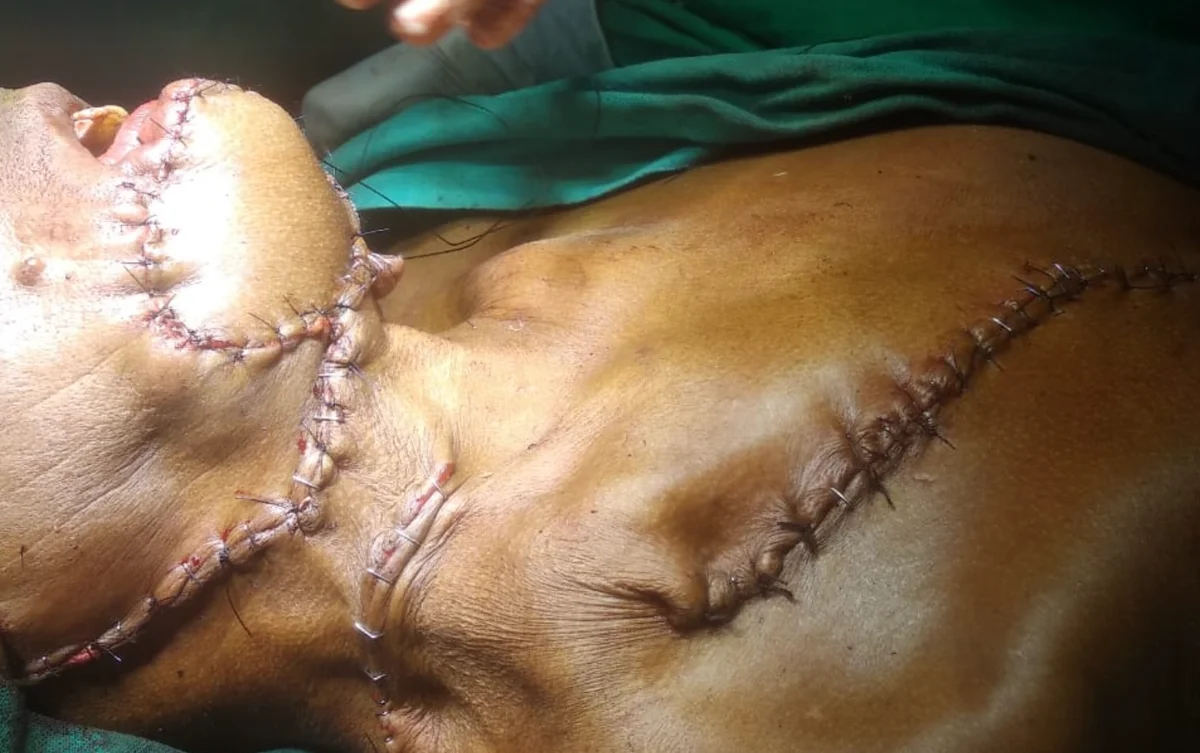
Selected cases managed by Dr. Abhisek Chatterjee. All images used with patient consent.

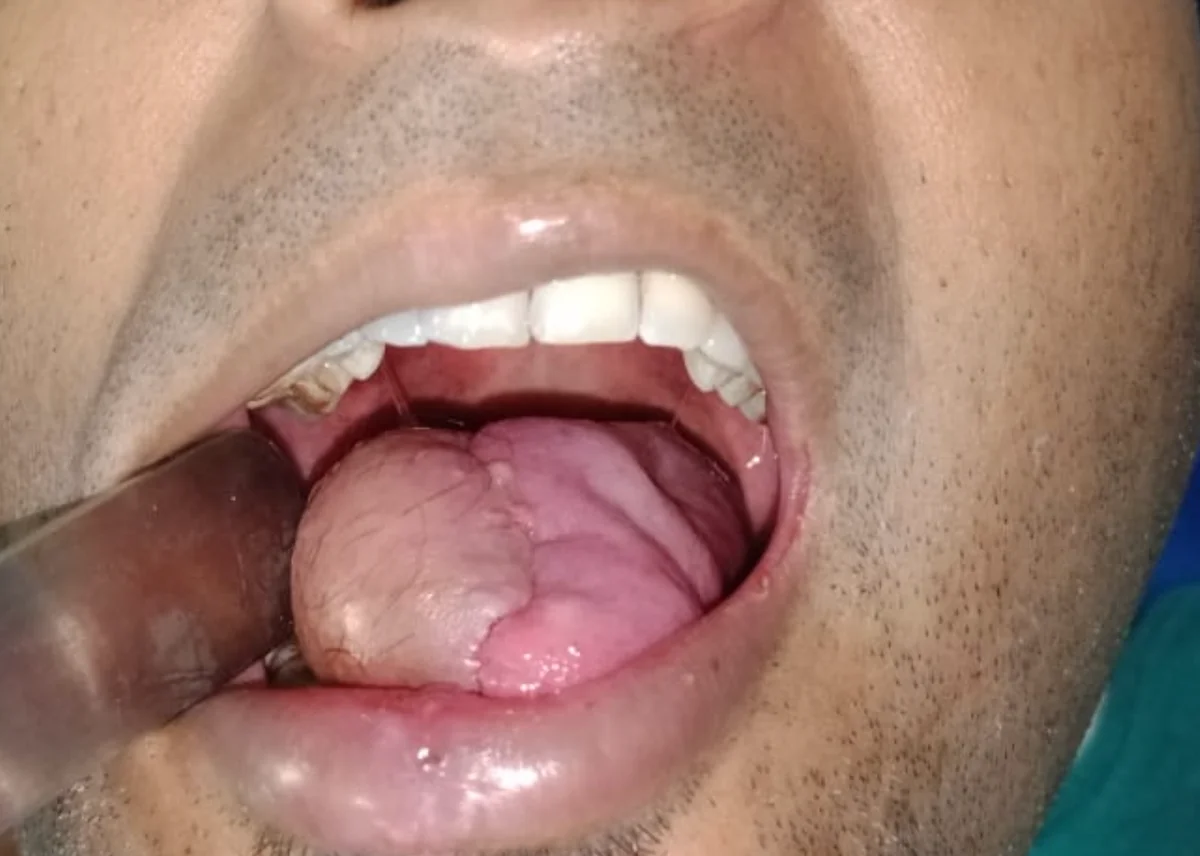
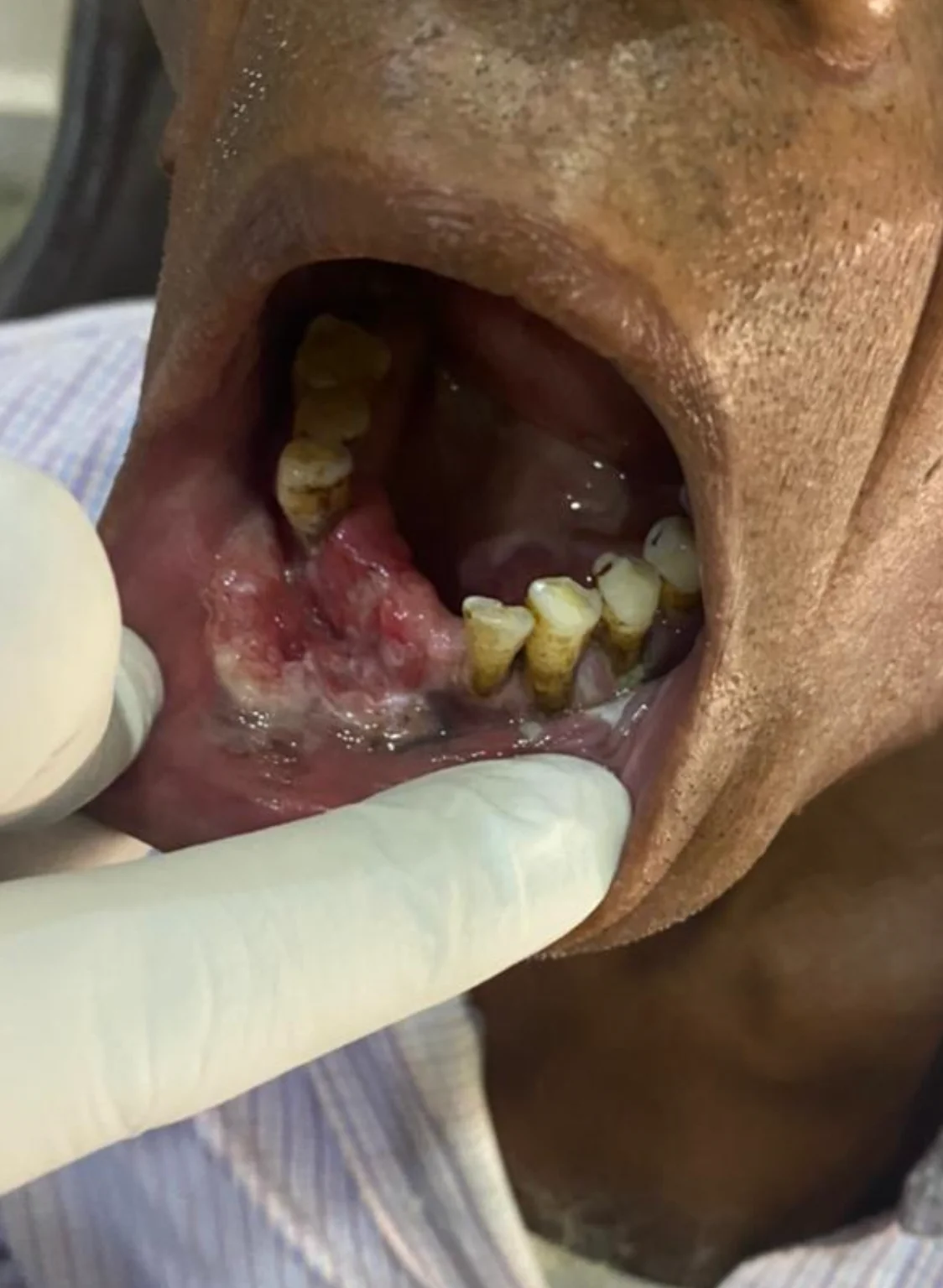

Do not delay. A non-healing mouth ulcer, white patch, or neck lump lasting more than 3 weeks requires specialist evaluation. Book an appointment with Dr. Abhisek Chatterjee at Rampurhat today.